National incident declared as measles cases surge
Health chiefs have declared a national incident over a surge in measles cases amid fears that a West Midlands outbreak could spread.
The UK is on a trajectory for “everything getting much worse” when it comes to the virus spreading, the head of the UK Health Security Agency (UKHSA) has warned.
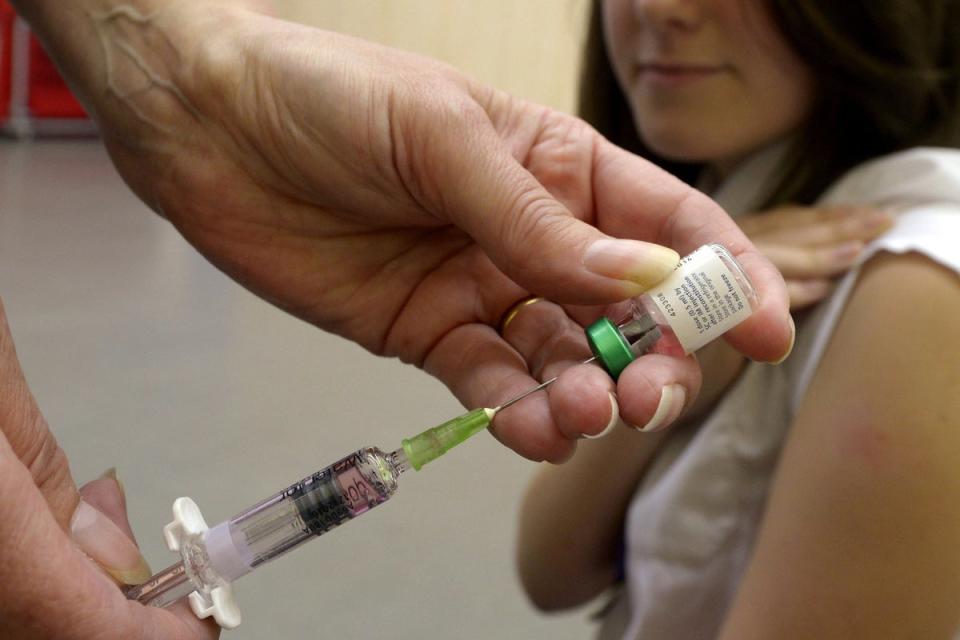
Professor Dame Jenny Harries said that without urgent action, measles is likely to spread rapidly and that immediate action was needed to boost uptake of the measles, mumps and rubella (MMR) vaccine in areas where numbers of children having the jab were low.
“We need a long-term concerted effort to protect individuals and to prevent large measles outbreaks,” she said.
Symptoms of the highly infectious virus include a bad rash, high fever, ear infections, red, watery eyes and aches and pains.
But official figures show uptake of the vaccine is at its lowest point in more than a decade.
In 2022-23, only 84.5 per cent of youngsters in England had received both doses of the jab by the age of five – the lowest level since 2010-11.
Since 1 October last year, there have been 216 confirmed measles cases and 103 probable cases in the West Midlands, according to the agency’s figures.
Four-fifths of cases were in Birmingham and one in 10 was in Coventry, most in children aged under 10.
In London, two councils have written to parents to tell them any unvaccinated child who comes into close contact with a measles case could be asked to self-isolate for up to 21 days.
Last year, there were 1,603 suspected cases of measles in England and Wales, a sharp increase from 735 cases the year before and 360 before that.
Declaring a national incident signals a growing public health risk and enables health chiefs to focus their resources in specific areas.
Dame Jenny said uptake of MMR vaccines differed among communities.
“This is an important point, I think, for the West Midlands, for those in Muslim communities. They will be not keen to take up one of the MMR vaccines that we offer which has a pork-based derivative.
“But it’s really important that they’re aware there is a non-porcine vaccine which is available to them and very effective.”
She added: “Children who get measles can be very poorly and some will suffer life-changing complications.”
False concerns linking the vaccinations to autism, which were later disproven, caused the uptake rate to drop during the late 1990s.
Helen Bedford, professor of children’s health at UCL Great Ormond Street Institute of Child Health, said: “About one in 1,000 people with measles develops inflammation of the brain, and even in high-income countries like the UK, about one in 5,000 die from the infection.
“Apart from managing the symptoms of measles, there is no treatment.”
NHS England has, for the first time, issued infection-control guidance on measles to the NHS.
It involves ensuring communication between GP surgeries and hospitals if a patient with measles is admitted for care.
A measles patient who needs to see a GP should be isolated at the time of arrival – for example, in a side room – and appointments should be scheduled to reduce waiting times in reception areas to avoid spreading the disease, the guidance says.


